For Men Who Refuse to Settle
Cure Prostate Cancer.
Keep Your Life.
Prostate cancer treatment doesn't have to mean diapers, impotence, or months of recovery. TULSA-PROTM offers a precise, MRI-guided alternative to surgery and radiation—one that eliminates cancer while preserving sexual function, bladder control, and dignity.
What is TULSA-PROTM?
An FDA-approved, MRI-guided ultrasound therapy that precisely ablates prostate tissue without incisions, without radiation, and without collateral damage to surrounding structures.

MRI-Guided Precision
Real-time monitoring with meticulous accuracy, protecting critical structures
Inside-Out Ablation
Treats from urethra outward, avoiding the rectum and neurovascular bundles
Single Session
One outpatient procedure, go home the same day

Function Preservation
Preserved urinary control and erectile function
TULSA-PROTM vs. Surgery
Traditional radical prostatectomy, whether open or robotic-assisted, requires incisions and physical removal of the prostate gland. TULSA-PROTM offers a fundamentally different approach with superior functional outcomes.
-
No Incisions Required
TULSA-PROTM: Transurethral approach, completely incision-free
Surgery: Major surgery with incisions (open or robotic) and additional risks -
Erectile Function Preservation
TULSA-PROTM: 98% preserved (focal), 87% at 5 years (whole-gland)
Surgery: 30-70% preserved -
Continence Preservation
TULSA-PROTM: 98% maintained, 92% pad-free at 5 years
Surgery: 60-90% maintained -
Recovery
TULSA-PROTM: Days to resume normal activities
Surgery: Weeks to months -
Hospital Stay
TULSA-PROTM: Outpatient, same-day discharge
Surgery: 1-2 days typical
TULSA-PROTM vs. Radiation
Radiation therapy typically requires 20-40 treatment sessions over several weeks with cumulative radiation exposure. TULSA-PROTM delivers a single-session treatment with no radiation and improved functional outcomes.
-
Treatment Duration
TULSA Pro: Single session (1-3 hours), same-day discharge
Radiation: 5-40 sessions over 4-8 weeks -
Radiation Exposure
TULSA Pro: None - ultrasound-based therapy
Radiation: Cumulative radiation exposure with long-term risks -
Erectile Function Preservation
TULSA Pro: 98% preserved (focal), 87% at 5 years
Radiation: 40-60% preserved -
Continence Preservation
TULSA Pro: 97% maintained at 5 years
Radiation: 80-90% maintained -
Recovery
TULSA Pro: Minimal downtime, days to normal activities
Radiation: Weeks to months of daily treatment, years until late-risks show themselves
Proven Clinical Outcomes
Data from CAPTAIN, the world's first head-to-head TULSA vs. prostatectomy clinical trial, the pivotal TACT trial and pooled clinical studies demonstrate the effectiveness and safety of TULSA-PRO.
96%
PSA reduction
97%
Urinary continence maintained
87%
Erectile function preserved
97%
No urethral stricture
Key Clinical Findings
TACT Trial Results
- 96% of 115 men experienced PSA reduction of 75% or more at 12 months
- 79% of intermediate-risk patients free of Gleason Group 2+ disease at 12-month biopsy
- No rectal injuries or Grade 4 adverse events reported
4-Year Follow-Up Data
- 81% of previously potent patients reported erections sufficient for penetration
- 94% pad-free continence, 99% socially continent at 4 years
- 22% required salvage therapy (TULSA-PROTM does not preclude further treatment)
The Journal of Urology, Vol 209, No 4S, May 2023

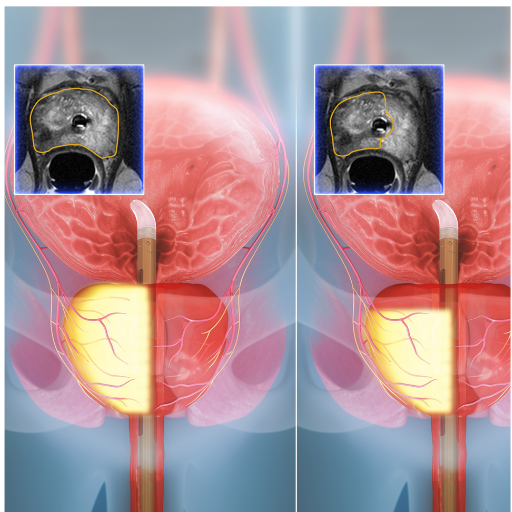
CAPTAIN Trial
The World's First Head-to-Head Comparison of TULSA-PROTM vs. Robotic Prostatectomy (RP)
- Significantly Less Blood loss: TULSA mL vs. RP 100 mL, p<0.001.
- Significantly Shorter Hospitalization: TULSA 0.29 days vs. RP 1.24 days, p<0.001.
- Significantly Less Pain: Numerical Rating Score lower TULSA vs. RP to post-treatment day 6, p<0.05.
- Significantly Better Quality of Life: Higher overall health scores TULSA vs. RP for all 30 days measured after treatment, p<0.05. Less extreme problems or mobility issues (0% for TULSA vs. 12% for RP, p=0.001), self-care (3% for TULSA vs. 17% for RP, p=0.005), and usual activities (17% for TULSA vs. 40% for RP, p=0.008).
Urologic Oncology, Vol 43, Issue 3, March 2025
How TULSA-PROTM Works
A precise, four-step process guided by real-time MRI imaging
1

Device Insertion
The ultrasound applicator is inserted into the urethra, along with a cooling device to protect surrounding tissue.
2

MRI Visualization
Real-time MRI provides clear views of the prostate and critical structures for precise planning.
3
Custom Planning
Dr. Hong customizes treatment boundaries based on anatomy and areas to treat or spare.
4

Precision Ablation
The system delivers therapeutic ultrasound within prescribed boundaries while monitoring in real-time.
Ready to Learn More?
Don't settle for outdated options. If you've been told surgery or radiation are your only paths forward, it's time for a second opinion—one grounded in precision, experience, and respect for your life after cancer.